
OSI: Your Trusted Partner for Accurate Insurance Verifications and Authorizations
Insurance verification is a crucial process in a healthcare practice to confirm the coverage and benefits of a patient’s insurance plan before providing medical services. Certain medical treatments need to be approved or pre-certified prior to being performed so that they are covered by the insurance company. Managing insurance verifications and authorizations could be a tedious and time-consuming task for busy practices.
At OSI, we understand that identifying patient benefits and coverage for specific medical procedures prior to the point of service is crucial to mitigate risks such as payment delays, resubmission issues, errors, or claim denials.
Our professional insurance verification specialists can efficiently handle this time-intensive task. Our clients include major insurers in the country such as Blue Cross Blue Shield, United Healthcare, AETNA, and GHI. With our insurance authorization services, your practice can stay up-to-date with insurance regulations and guidelines.
Benefits of Insurance Verification and Pre-authorization
- Avoid payment delays
- Reduce claim denials
- Boost revenue
- Improve practice efficiency
- Reduce bad debts
- Enhance patient satisfaction

Specialties We Serve
- Anesthesiology
- Behavioral
- Cardiology
- Chiropractic
- Critical Care
- Dentistry
- Dermatology
- Endocrinology
- Family Practice
- Gastroenterology
- General Surgery
- Internal Medicine
- Neurology
- Obstetrics & Gynecology
- Orthopedic
- Physical Therapy
- Speech & Language Pathology
- View More
Dermatology
Endocrinology
Internal Medicine
Obstetrics & Gynecology
Speech & Language Pathology
Advantages of Partnering with OSI
Pre-certification and insurance verification services at OSI are comprehensive and thoroughly efficient. Importantly, you have no long-term yearly contracts to sign.
Here’s what we do:
- Call the carriers directly and verify the insurance details
- Document and record the calls thus saving crucial time for your practice
- Free up your staff from waiting on hold with insurance companies
- Work directly on your software or offline
- Work on your schedule and stay ahead of schedule
- Stay 3 to 5 days ahead of your schedule
You can:
- Hire a full time equivalent (FTE) and save on taxes and benefits
- Get regular reports on completed authorizations and/or status updates
- Enjoy 30% to 40% savings on operational costs
- Get an experienced person working on our account. No hiring or training

Patient Insurance Details We Verify
Our team verifies diverse details including:
Co-pays
Co-insurances
Claims mailing address
Deductibles
Patient policy status
Effective date
Payable benefits
Plan exclusions
Type of plan and coverage details
Referrals and pre-authorizations
Out-of-network benefits
DME reimbursement
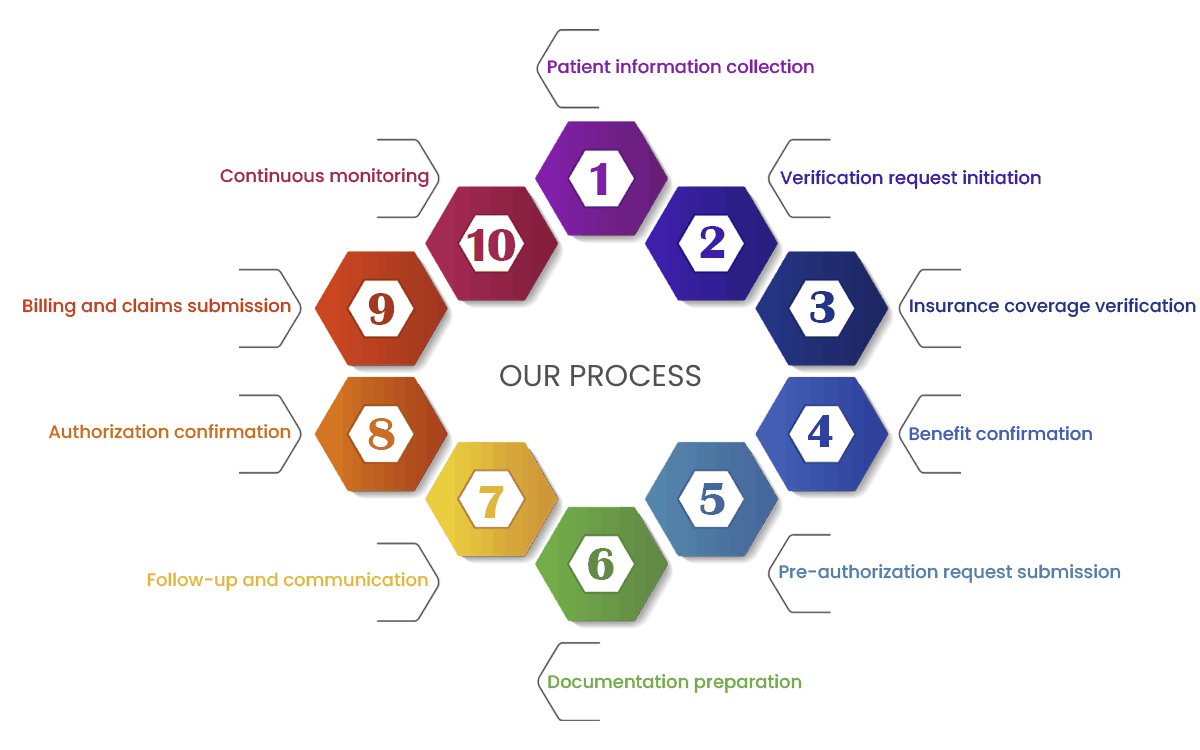
Our Patient Eligibility Verification and Authorization Process
We begin with the collection of patient details, initiating a thorough insurance verification process to provide a solid foundation for accurate claims processing. We navigate through the insurance landscape, verifying coverage details, assessing benefits, and strategically submitting pre-authorization requests to ensure a streamlined and efficient process.
Affordable & Flexible Pricing Plans
Fixed Cost Pricing
Like an FTE model, a person is dedicated to your practice. Perfect for a practice that is busy. They work as an extension to your business.
- A dedicated employee or team member
- This person or team can handle multiple responsibilities
- Preset pricing and production guidelines
- No Start-up fees
Per Transaction Pricing
Perfect for a practice that is unsure about their work requirements. This can have per request pricing for eligibility and other functions.
- Dedicated team or employee
- This person or team can handle multiple responsibilities
- A per transaction or hybrid model
- No Start-up fees
Experience effortless pre-authorizations with our expert services!
Call: (800) 670-2809
What Our Clients Say
FAQs
Why is insurance verification and prior authorization crucial for medical practices?
Pre-certification allows practices to secure approval for specific medical services in advance, enhancing financial planning, and ensuring a smoother reimbursement process.
How does the verification process contribute to patient satisfaction?
Can eligibility verification and pre-authorization be customized for different medical specialties?
How does your process ensure compliance with healthcare regulations?
Recent Posts
What Is the Difference between Insurance Verification and Insurance Authorization?
Suppose that you managed to provide exemplary patient care at your medical practice and your patients leave satisfied with the treatment received, leading to positive feedback and improved health outcomes. However, when you check to see the status of your claim...
Five Compelling Reasons to Outsource Dental Insurance Verification
In dental practices, insurance verification sets the stage for efficient revenue cycle management. According to a Dentistry IQ article, dental insurance checks make up approximately 50% of practice income. However, verifying dental insurance is a labor-intensive and...
How to Code and Bill for Mental Health Services
The National Institutes of Health (NIH) concluded that over 20% of Americans (57.8 million) live with some form of mental illness. Treatments include various forms of psychotherapy, medications, psychosocial interventions and other modalities such as electroconvulsive...



